Night sweats are one of the most common and most disruptive symptoms that women experience throughout their lives. While menopause gets most of the attention, hormonal night sweats can start much earlier than many women expect and can be triggered by a range of factors beyond just the menopause transition.
If you are a woman dealing with night sweats, this guide covers everything from the hormonal causes to practical solutions, including what actually works for managing them day to day.

Why Do Women Get Night Sweats?
Women are more prone to night sweats than men, primarily because of the hormonal fluctuations that occur throughout a woman's life. Oestrogen plays a direct role in how the hypothalamus (the brain's thermostat) regulates body temperature.
When oestrogen levels shift, whether up or down, the hypothalamus can become hypersensitive to temperature changes and trigger sweating in response to very minor fluctuations that it would normally ignore.
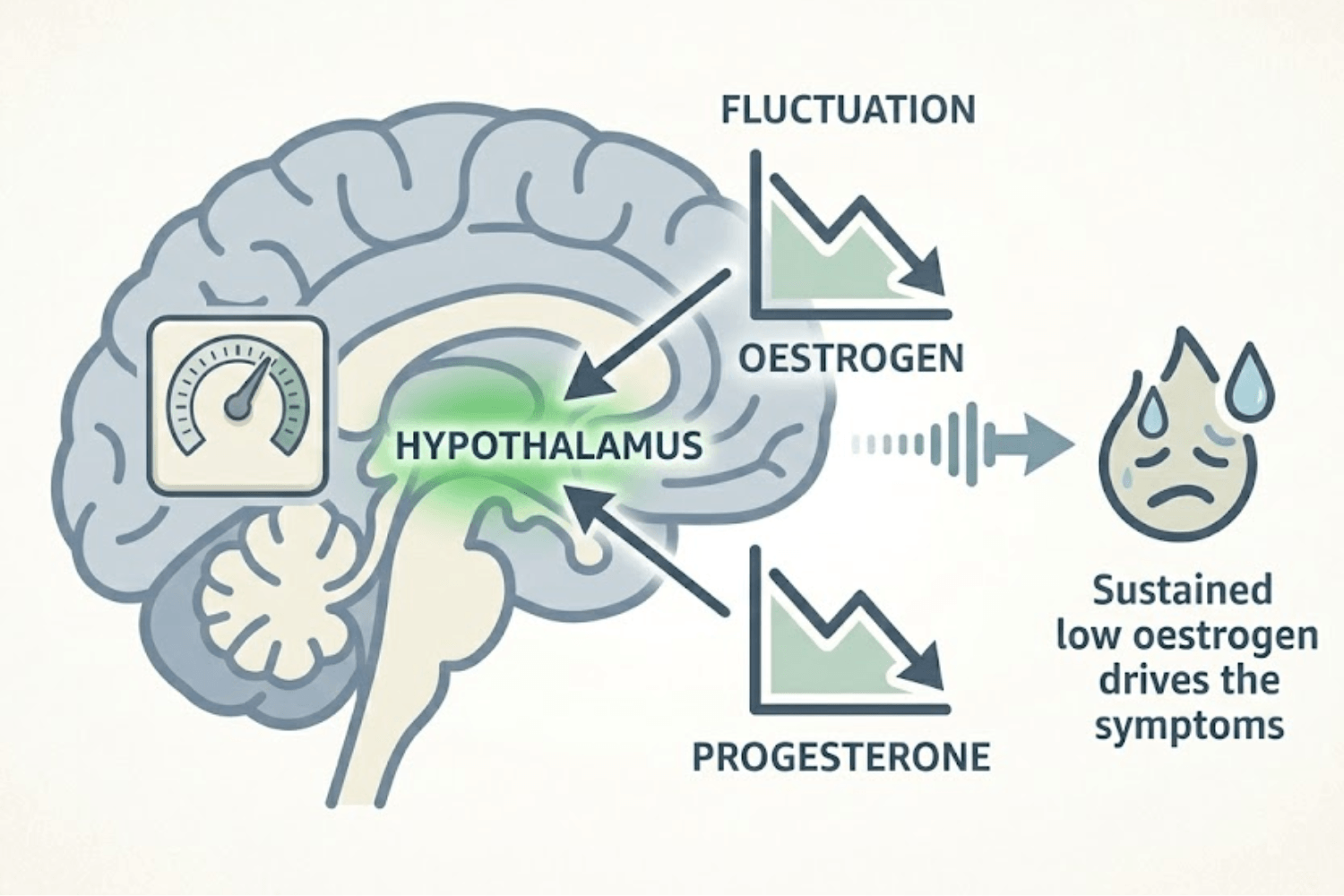
This means night sweats can occur during several different life stages: before your period, during pregnancy, after giving birth, during perimenopause, and through menopause. They can also be caused by the same non hormonal factors that affect everyone, including stress, medications, alcohol, and underlying health conditions.
Night Sweats Before Your Period
Many women notice that they sweat more at night in the few days before their period starts. This happens because of the hormonal changes that occur during the luteal phase of your menstrual cycle, the phase between ovulation and the start of your period.
After ovulation, progesterone levels rise significantly, which slightly raises your basal body temperature. In the days before your period, both progesterone and oestrogen drop sharply, and this hormonal shift can trigger the hypothalamus to respond with hot flushes and sweating, particularly at night.
Premenstrual night sweats are usually mild compared to menopausal sweats and tend to resolve once your period starts. If they are particularly severe or disruptive, it is worth mentioning to your GP, as they can sometimes be connected to premenstrual dysphoric disorder (PMDD) or other hormonal issues.
Perimenopause and Night Sweats
Perimenopause is the transition phase leading up to menopause, and it can begin years before your periods actually stop. Most women enter perimenopause in their mid 40s, but it can start as early as the late 30s.
During this time, your hormone levels start to fluctuate unpredictably, and night sweats are often one of the first symptoms women notice.

Perimenopausal night sweats can be confusing because your periods may still be regular (or at least semi regular), so you might not immediately connect the sweating to hormonal changes. You might assume it is stress, or your bedroom, or something you ate. But if you are in your late 30s or 40s and have started sweating at night when you did not before, fluctuating oestrogen is a likely explanation.
Sweating around the neck and chest area is particularly common during perimenopause. This area has a high concentration of both sweat glands and blood vessels near the surface of the skin, which makes it especially responsive to hormonal triggers. If you have noticed that your neck and chest are where you sweat the most at night, you are not imagining it, and you are certainly not alone.
Night Sweats During Menopause
Menopause itself is defined as the point when you have gone 12 months without a period. By this stage, oestrogen levels have dropped significantly and permanently, and this sustained low oestrogen is what drives the most intense and persistent night sweats.
Research consistently shows that around 75% of women experience hot flushes and night sweats during the menopausal transition, with approximately 30% experiencing severe symptoms.
A study of over 10,000 postmenopausal women published in BJOG found that more than half were still experiencing symptoms an average of 10 years after their last period, and around 40% of women aged 60 to 65 still report ongoing hot flushes and night sweats.
The severity varies enormously from person to person. Some women have mild sweats that are more of an inconvenience, while others experience drenching episodes that soak through nightclothes and bedding, sometimes multiple times per night.
Menopausal night sweats tend to follow a pattern. You might feel a sudden wave of heat that starts in your chest or face and spreads outward, followed by intense sweating, and then often a chill as the sweat evaporates and your body overcools. This whole cycle can happen in a few minutes, but the disruption to your sleep lasts much longer.
How Long Do Menopausal Night Sweats Last?
This is one of the most common questions women ask, and unfortunately the answer is not as reassuring as most people hope. The SWAN study, which tracked over 3,300 women from diverse backgrounds, found that the median duration of vasomotor symptoms was 7.4 years.
Women who started experiencing symptoms before their periods stopped had them for an average of 9 to 10 years. When symptoms did not begin until after the final menstrual period, the average duration was around 3.5 years.
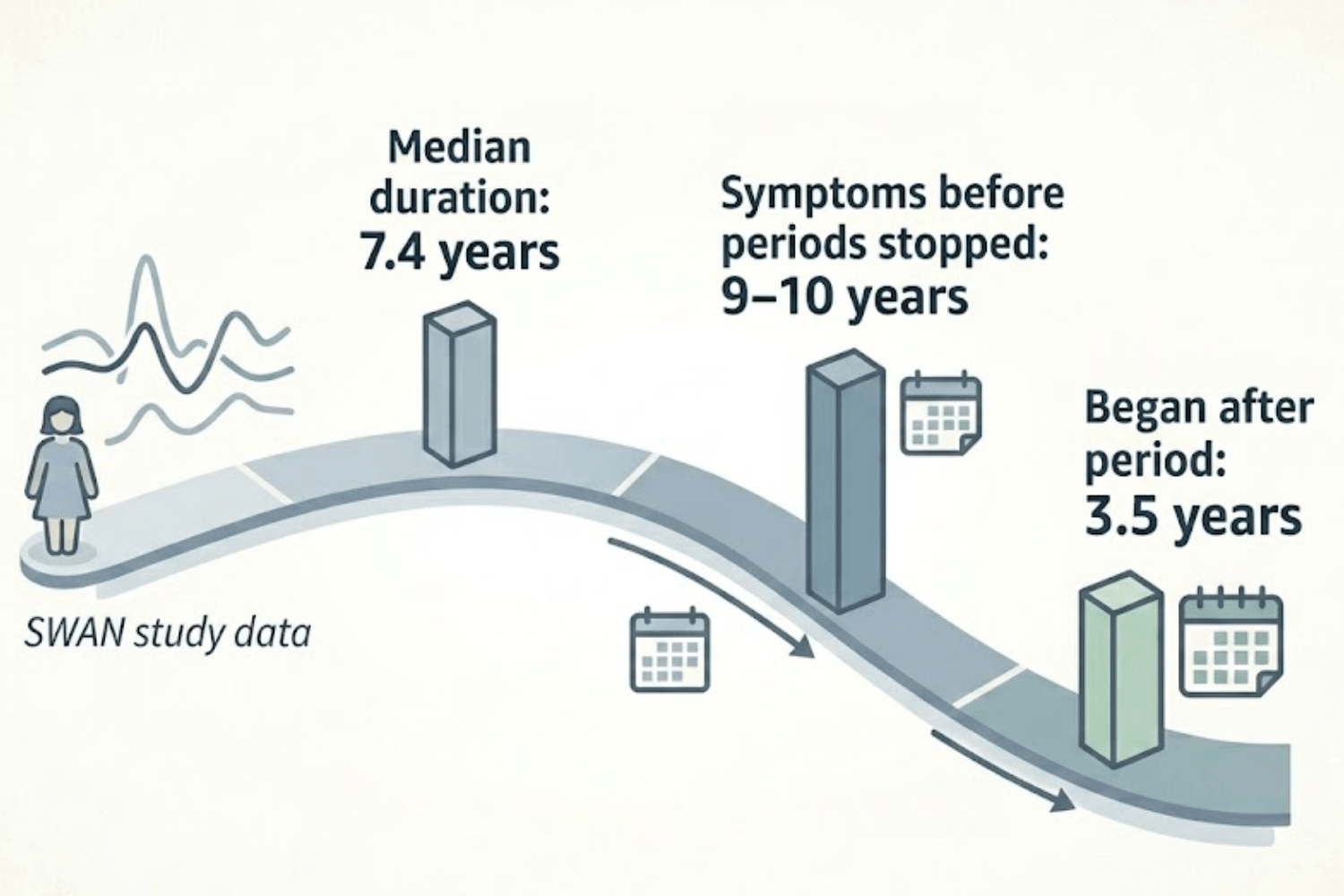
About 14% of women experience symptoms for over a decade, and around 20% have symptoms lasting 15 years or more. For some women they resolve within a year or two, while others experience them for a decade or more.
The duration tends to be longer for women who start experiencing hot flushes early in their menopausal transition. The SWAN study also revealed significant variation by ethnicity: African American women experienced the longest duration of symptoms (averaging over 11 years), while Japanese and Chinese women had symptoms for approximately half that time.
Women who were current or former smokers, overweight, stressed, depressed, or anxious also reported longer durations, and for women from certain ethnic backgrounds. Research has also shown that women who are under significant stress or who have a higher body weight tend to experience more prolonged symptoms.
The important thing to take from this is that menopausal night sweats are not something you should just grit your teeth and endure. Given that they can last for years, investing in proper management, whether through medical treatment, lifestyle changes, or both, makes a real difference to your quality of life.
HRT, CBT and Medical Options
Hormone replacement therapy (HRT) is the most effective medical treatment for menopausal night sweats, with research showing it can reduce vasomotor symptoms by up to 75% to 90% in some cases. It works by replacing the oestrogen that your body is no longer producing, which directly addresses the root cause of the sweating.
HRT is available in several forms including tablets, patches, gels, and sprays, and your GP can help you find the right type and dosage.
HRT is not suitable for everyone, and it does come with some risks that your doctor will discuss with you. But for many women, the benefits significantly outweigh the risks, especially when night sweats are severely affecting sleep and daily life.
Cognitive behavioural therapy (CBT) is another option that has gained recognition in recent years. In November 2024, NICE updated its menopause guidance to recommend CBT alongside or as an alternative to HRT.
CBT for menopause focuses on changing the thought patterns and behaviours that can amplify symptoms, including night sweats. It includes developing calming routines, managing the anxiety that night sweats create, and changing sleep behaviours that make symptoms worse.
Other medical options include certain antidepressants (at low doses, specifically for managing hot flushes), clonidine, and gabapentin. These are typically used when HRT is not suitable. Your GP can advise on the best option for your situation.
Natural Remedies for Menopausal Night Sweats
Many women look for natural alternatives to manage night sweats, either because they cannot take HRT or because they prefer to try non pharmaceutical options first.
Sage supplements are one of the most commonly used herbal remedies for menopausal sweating, and there is some evidence that sage extract can reduce the frequency and intensity of hot flushes.

Black cohosh is another popular option, though the research on its effectiveness is mixed. Evening primrose oil, red clover, and St John's Wort are also frequently mentioned, but the evidence for these is limited.
It is important to approach natural remedies with realistic expectations. None of them are as effective as HRT for reducing night sweats, and some can interact with medications. If you are considering herbal supplements, it is worth discussing them with your GP or pharmacist first, especially if you are taking any other medications.
The lifestyle changes covered in our how to stop night sweats guide, including bedroom temperature, diet, exercise, stress management, and choosing the right bedding, are often more impactful than herbal remedies and have no side effects.
The Best Bedding for Menopause Night Sweats
If you are sweating through your sheets multiple times a week, your bedding choices matter enormously. The wrong bedding turns a bad situation into a miserable one, while the right bedding can genuinely improve your comfort even on your worst nights.
Natural fabrics are essential. Bamboo bedding is one of the best options for menopausal night sweats because it is highly breathable, wicks moisture away from your skin, and is naturally antibacterial.

Eucalyptus bedding offers similar benefits with an especially silky feel. Both are significantly better than cotton for moisture management, and leagues ahead of any synthetic material.
We have put together a dedicated collection of bedding for the menopause that brings together the products specifically designed to help with night sweats and temperature regulation. For a full breakdown of fabrics, duvets, pillows, and what to avoid, see our guide on the best bedding for night sweats.
Keeping Your Sleep Environment Fresh
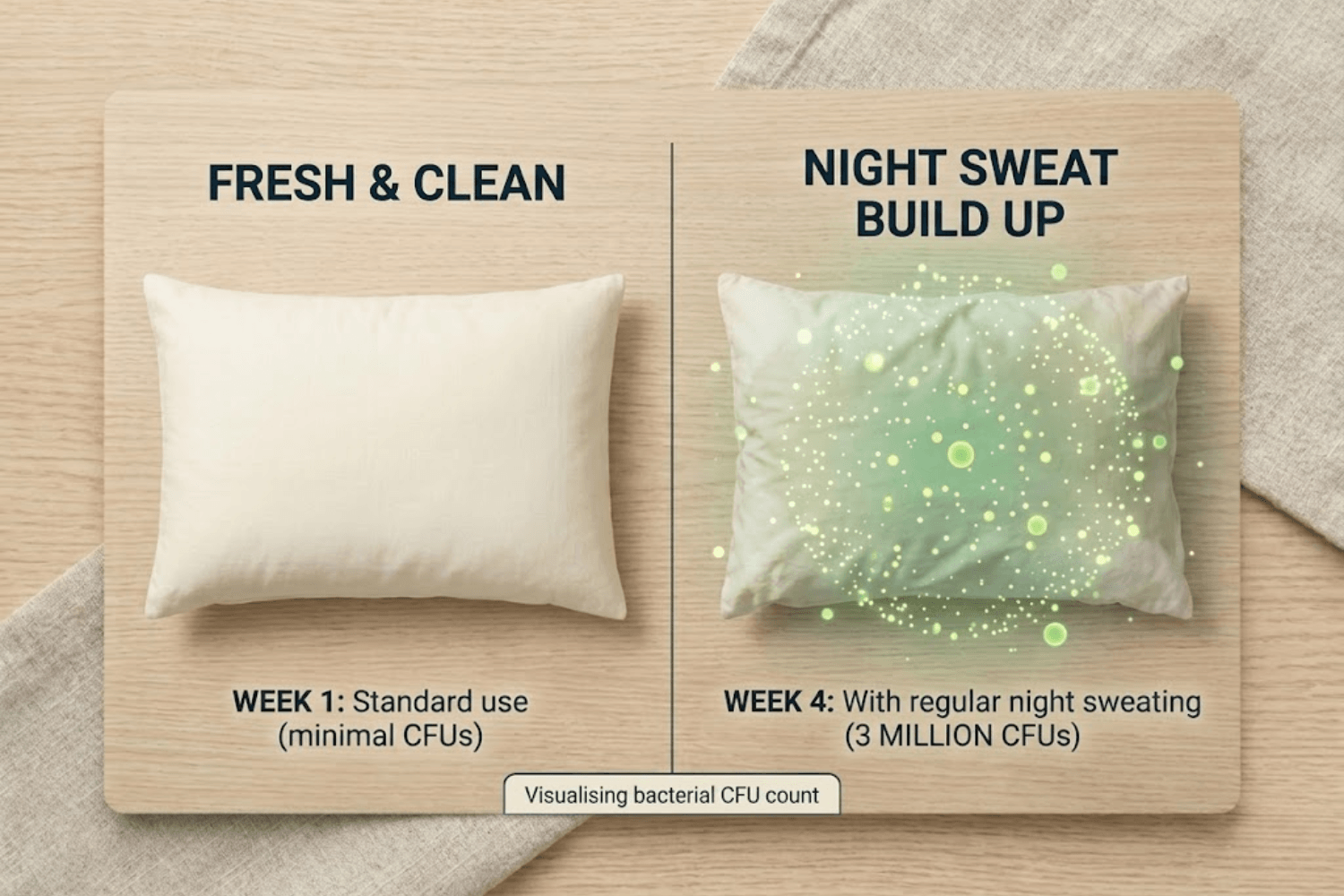
When you are sweating through your bedding regularly, freshness becomes an ongoing challenge. You wash your sheets, they feel lovely for a night or two, and then the sweat buildup starts again. The bacteria that thrive in warm, damp conditions begin to multiply, and before the week is out your bedding can start to feel stale and smell off.
A daily maintenance routine helps enormously. Pull your duvet back every morning to let your bedding air out and dry. If you can, open a window. Then use a bedding hygiene spray to keep the bacteria in check between washes.

It is a small daily habit that makes a disproportionate difference to how your bed feels at the end of the day. A silk sleep mask is also worth considering if you use one. Silk is naturally cooling and will not trap heat against your face the way synthetic masks do, which can be a real relief during a hot flush.
Sweating Around the Neck and Chest at Night
This is one of the most commonly searched symptoms among women experiencing night sweats, and for good reason. Sweating that is concentrated around the neck, chest, and upper back is particularly common during hormonal changes, and it can be one of the most uncomfortable patterns because these areas are in close contact with your pillow and sheets.
The reason this area is so affected is partly anatomical (high concentration of sweat glands and blood vessels near the skin surface) and partly hormonal (oestrogen receptors in this area make it particularly responsive to hormonal fluctuations).
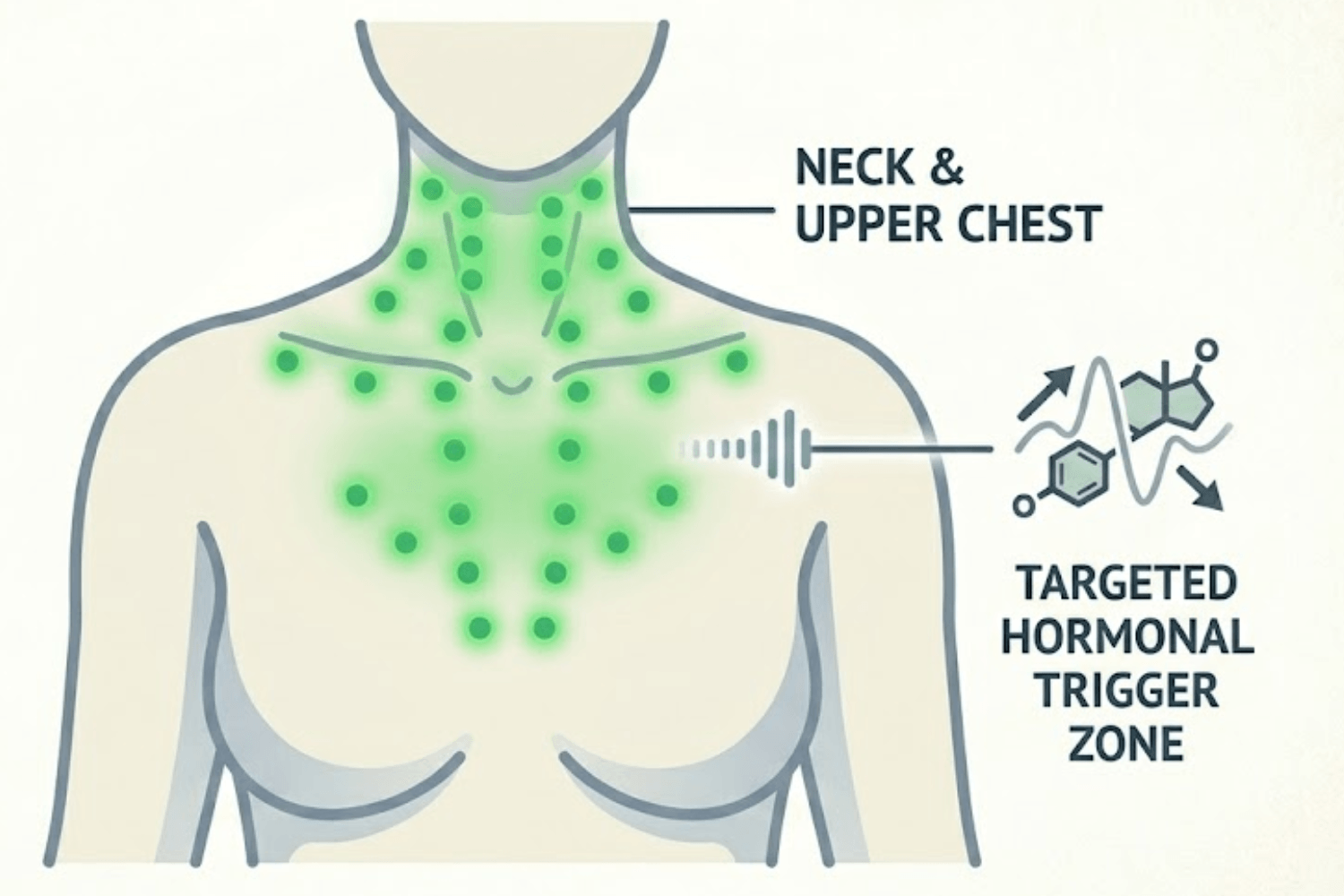
Practical tips for managing neck and chest sweating include keeping your hair off your neck during sleep, using a breathable pillowcase (bamboo or silk), wearing a loose low neckline to bed rather than a high collar, and keeping a small hand towel nearby to pat dry if you wake up sweating.
The daily bedding spray routine is especially important here, as the area where your neck meets the pillow tends to be the first place that bacterial buildup creates an unpleasant smell.